Update, 12:20 p.m. October 20: The San Francisco Department of Public Health has announced it will end the city’s state of emergency around monkeypox (MPX) on October 31.
SF health officials said that MPX cases “have slowed to less than one case per day,” and that more than 27,000 city residents have now received the MPX vaccine.
San Francisco originally declared this public health emergency for MPX back in July, and was the first U.S. city to do so.
Original post:
A note: Several public health organizations, including the California Department of Public Health, have chosen to refer to monkeypox as “MPX” (pronounced “em-pox”) with the aim of reducing homophobic and racial stigma surrounding the virus. For the rest of this story, we use “MPX” for these reasons, except in direct quotes or other cases where it would confuse readers.
Back on August 4, the White House declared MPX a public health emergency. At the time of this announcement, there were more than 6,616 cases reported in the U.S.
As of Sept. 14, the CDC now reports 22,630 cases nationwide. And because of limited testing, this figure most likely still represents something of an undercount.
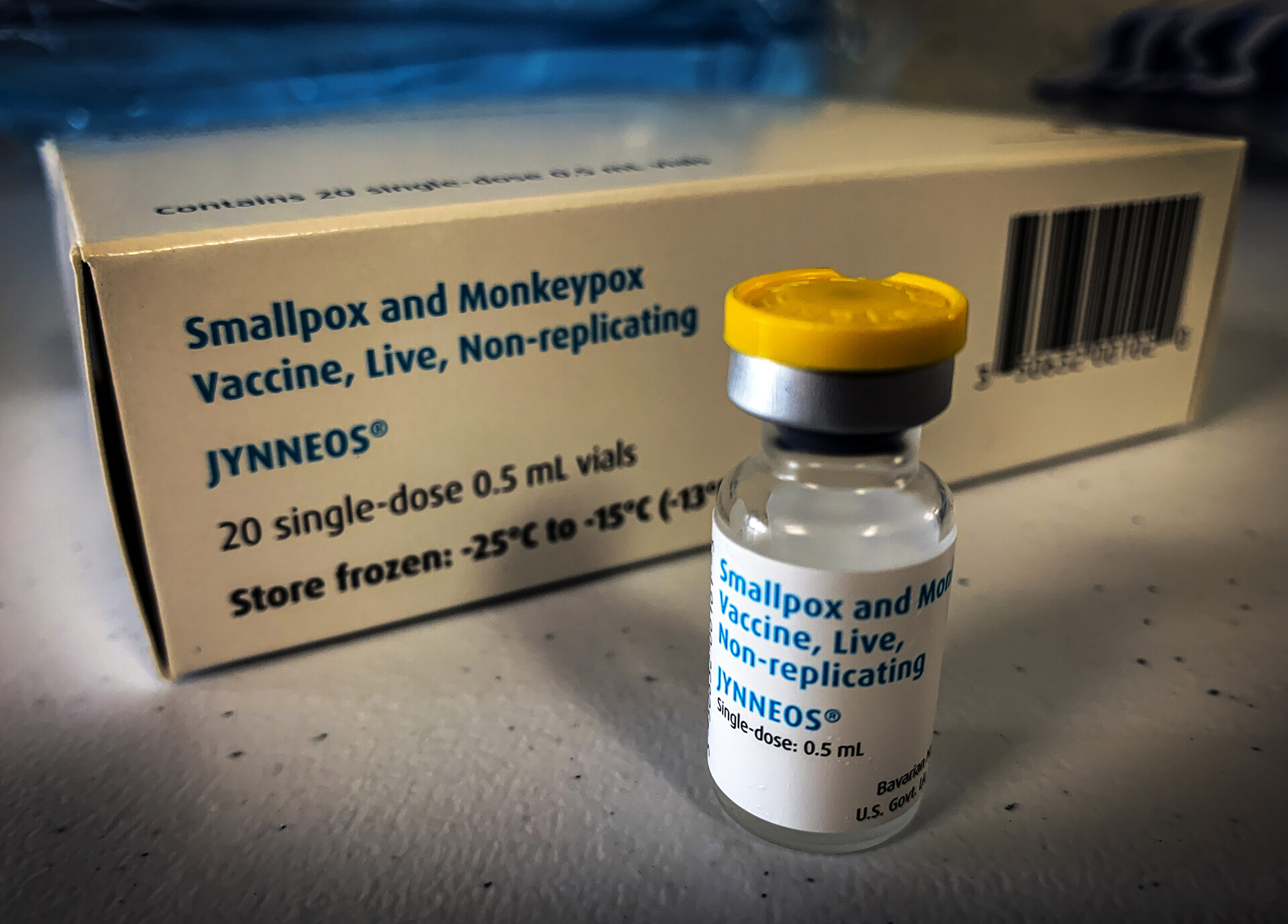
- Looking for where to find an MPX vaccine near you? Read our full guide to the MPX vaccine in the Bay Area.
“We are prepared to take our response to the next level in addressing this virus and we urge every American to take monkeypox seriously,” Health and Human Services Secretary Xavier Becerra said. Read more about what the public health emergency means.
On August 1, Gov. Gavin Newsom declared a State of Emergency over the MPX outbreak in California. A week prior, San Francisco had declared its own state of emergency over MPX. State and local health officials have affirmed that cases are rapidly rising and have asked the federal government to make MPX vaccines more widely available.
Jump to a specific answer:
- What are the symptoms of MPX?
- How many MPX cases are in the Bay Area?
- What should I do if I think I have MPX?
- How can I prevent being infected with MPX?
MPX has existed for decades — the first case among humans was registered in 1970 — but we’re now seeing multiple outbreaks across the U.S. See how many cases have now been reported nationwide according to the Centers for Disease Control and Prevention.
The majority of infections have been detected among gay and bisexual men, but public health experts have made it clear that MPX is an “equal opportunity disease,” meaning that anybody, regardless of sexual orientation, race, class or other demographic categories, is susceptible to infection.
However, public health organizations that serve the LGBTQ+ community in the Bay Area are still advising residents to learn more about MPX and how it spreads, particularly in the context of large public events in San Francisco celebrated by the queer community like Pride (the weekend of June 25), Dore Alley Weekend (the weekend of July 30) and Folsom Street Fair (the weekend of September 24) that take place in the summer and fall. San Francisco formally declared the outbreak a public health emergency back on July 28.
KQED spoke to physicians, public health officials and LGBTQ+ health groups to create this guide that includes the latest information on the disease, its transmission and available treatment, and what to do if you become infected. And if you’re looking for vaccine details specifically, you can read our full guide to where to find a MPX vaccine near you.
What is MPX?
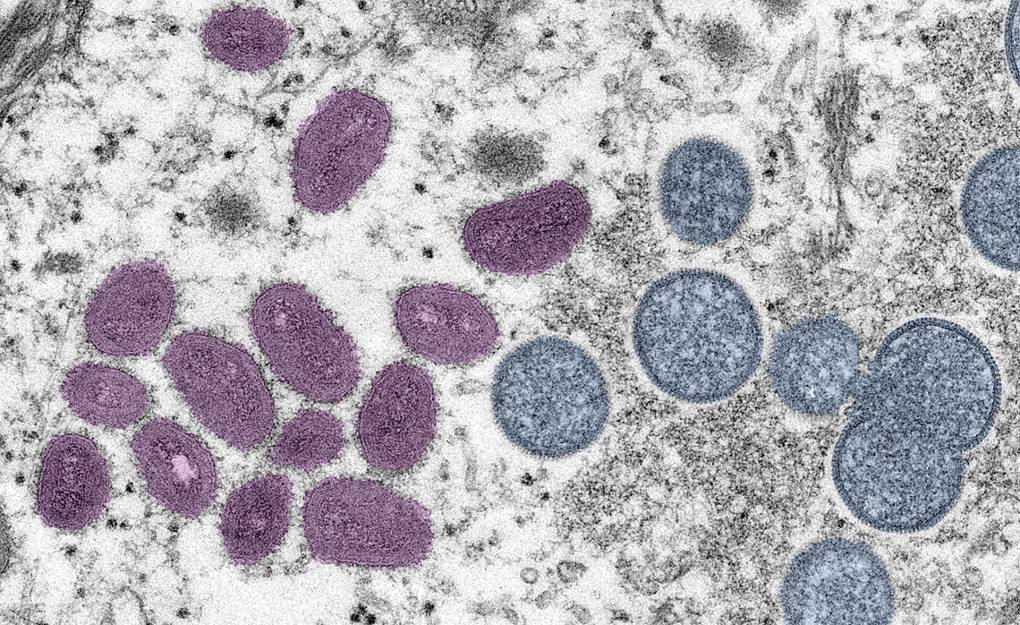
MPX is a disease that is caused when a person is infected with the MPX virus. As the name might suggest, the virus is related to the smallpox virus but it’s generally less severe and “much less contagious” than smallpox, according to the California Department of Public Health (CDPH).
Although you might assume MPX is also related to chickenpox, it’s not.
How did MPX get its name?
The disease was called “monkeypox” because it was first found in 1958 in monkeys. The Centers for Disease Control and Prevention say that the first human case of MPX was recorded in 1970.
Several public health bodies, including the California Department of Public Health and the San Francisco Department of Public Health, have now chosen to refer to the virus as “MPX” to address concerns that the original name furthers both racist and homophobic stigma around the disease and those who contract it.
In speech, MPX is usually pronounced “em-pox,” or the initials “em-pee-ecks.”
You may often see “monkeypox” on first usage, and “MPX” thereafter throughout an article or a resource from a public agency. Some official resources may also use “MPOX”. Rest assured these names are referring to the same disease.
How dangerous is MPX?
While it’s less severe than smallpox, MPX can still be a serious disease. The good news is that according to the CDC, MPX is “rarely fatal” — and that “over 99% of people who get this form of the disease are likely to survive.”
However, “people with weakened immune systems, children under 8 years of age, people with a history of eczema, and people who are pregnant or breastfeeding may be more likely to get seriously ill or die.”
Being sick with MPX typically lasts 2-4 weeks. The symptoms of MPX are similar to smallpox symptoms, but luckily are milder.
How many MPX cases are in California and the Bay Area right now?
See the number of probable and confirmed MPX cases reported in California right now, via the California Department of Public Health.
See the current number of probable and confirmed cases of MPX in San Francisco, via the San Francisco Public Health Department.
See the number of nationwide MPX cases state-by-state, according to the CDC’s map.

What are the symptoms of MPX?
According to the World Health Organization, the incubation period of MPX— that is, the amount of time between getting infected with MPX and actually developing the symptoms — is usually from six to 13 days. It can, however, range from five to 21 days.
The CDC says that you aren’t contagious during this incubation period.
After that initial incubation period, a person who’s infected with MPX will start to develop symptoms and become contagious to others. The CDC says that symptoms of MPX can include:
- A rash (also known as lesions) that can look like pimples or blisters that appears on the face, inside the mouth, and on other parts of the body, like the hands, feet, chest, genitals or anus. The rash goes through different stages before healing completely.
- Fever
- Headache
- Muscle aches and backache
- Swollen lymph nodes
- Chills
- Exhaustion
Much like with COVID, symptoms can present quite differently in different people. According to the CDC, some people get a rash first, and other symptoms follow. Other folks will only experience the rash itself.
The symptoms of MPX that aren’t the rash — like chills, fatigue and headache — are similar to symptoms of COVID. This means it’s entirely possible you could initially mistake a MPX infection for a COVID infection (or you could assume it’s another illness entirely, if you then test for COVID and get a negative result). This is why watching out for a rash is really important.
The San Francisco Department of Public Health says that usually, that MPX rash will start in the form of red, flat spots, which then become bumps. The bumps then become filled with fluid, which will then break and crust over into a scab.
In addition to the itch they can cause, MPX lesions can be very painful, especially in genital areas or the anus. The CDC notes that people also can have permanent scarring after the rash.
The symptoms of MPX can last two to four weeks. This means that, with an incubation period that could be as short as five days or as long as 21 days, a person could be dealing with an MPX infection for anywhere from under three weeks to almost two months.
Who can get MPX?
Anyone can get MPX.
As more details emerge of the outbreak in the U.S., it appears that MPX infections are particularly affecting communities of gay and bisexual men, and men who have sex with men.
The World Health Organization notes that trans people and gender-diverse people “may also be more vulnerable in the context of the current outbreak.”
San Francisco Health Officer Susan Philip says that LGBTQ+ folks currently being at higher risk for MPX has “nothing to do with sexual orientation or gender identity,” but is more about “being part of these networks and having close contact within those networks.” People in these networks “will likely then have expanded eligibility, expanded access to [an MPX] vaccine,” she says.