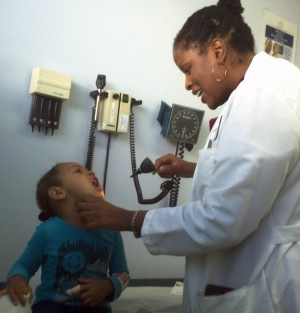
Dr. Mack has treated Sania since she was a baby and knew her well enough to realize that this bout of anemia was not serious. But she said that wouldn’t necessarily be the case for kids who aren’t covered for early pediatric care. “It could be a sign of something more ominous than it is, and we wouldn’t know that unless I saw her on a regular interval,” says Mack. “The AAP, the American Academy of Pediatrics, recommends certain lab tests drawn at certain intervals so we can catch these things.”
Under the Affordable Care Act, children who are on Medi-Cal, like Sania, will continue to have the full range of coverage recommended by the AAP. Children whose families have slightly more income and qualify for coverage under the new insurance Exchange will likely get significantly better benefits than they have now, but those benefits may not be equal to those under Medi-Cal.
The federal law outlines the so-called essential health benefits that insurers in the state Exchanges must cover. Each state must pick an existing insurance plan as a model -- a plan that has equivalent benefits to a "typical" employer plan. California was among the first states to pick its model benchmark.
“It’s a huge step forward for children’s health,” says Kelly Hardy, director of health policy at Children Now, a statewide advocacy group. California chose as its benchmark a Kaiser Small Group plan. That is the baseline plan, and there will be more expensive plans to trade up to, if people want to pay for more benefits. Although Kelly rejects the idea of one-size-fits-all insurance, she says state lawmakers did expand on the Kaiser plan to meet some of children’s needs.
“We’re really pleased that the legislature chose to add strong vision and comprehensive dental benefits for children,” says Kelly. “Those are two additions that are really important." (By comparison, people with employer-based health insurance often have separate insurance plans for dental and vision coverage.)
Yet children’s advocates like Hardy did not get everything they hoped for. Most importantly, she says, they did not convince state lawmakers to adopt the EPSDT for children insured through the state's Exchange. Hardy says that wasn’t practical to include for all kids because it’s simply too expensive. She also noted that many private plans, employer-based health insurance plans included, may not meet that standard.
Many pediatricians say that in reality, even the AAP standard is minimal coverage, especially for children with special needs such as asthma, Down syndrome or heart disease. As east bay physician Dr. Thomas Long puts it, “Is it the floor or is it the ceiling? We think it’s the floor, and the least we can do for all children.”
Dr. Long is an expert on child health financing with the American Academy of Pediatrics. He says the new Exchange’s standard of care falls short on things like mental health benefits, access to pediatric specialists and other needed coverage.
Insurers respond that the Exchange benefits package is broad enough -- and is certainly an improvement for children who have no or very limited insurance now. Charles Bacci, with the California Association of Health Plans, says there’s always a tradeoff between coverage and cost. “The more broad the benefit package, the more expensive your healthcare premiums are,” says Bacci. “The more narrow the benefit, the more affordable your premiums are.”
So the irony is that children on Medi-Cal, including half a million new enrollees under the Affordable Care Act, may have the broadest coverage, while children from slightly higher income families in the Exchange, may have at least somewhat narrower benefits. But, says Bacci, if the half-million new kids in the Exchange were also guaranteed the best coverage, healthcare costs would explode.
Support for this report came from the Lucile Packard Foundation for Children’s Health Journalism Fund, a program of the USC Annenberg School of Journalism’s California Endowment Health Journalism Fellowships.