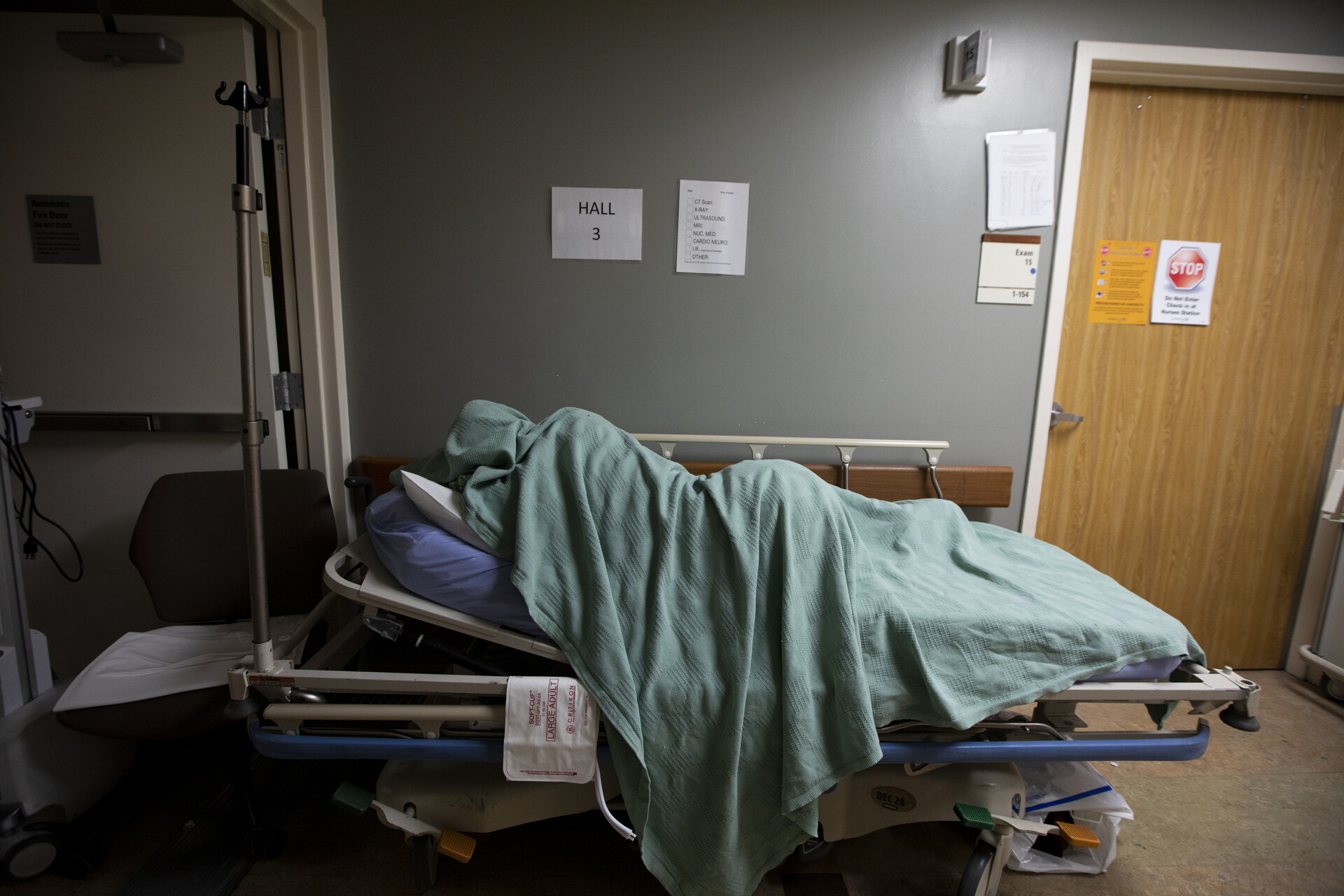
It’s not uncommon for really sick patients to wait three, four or even five days for a transfer, Marks said.
UC Davis Medical Center turned down more than 9,900 transfer requests in a little over a year due to limited capacity, The Los Angeles Times reported. And, a spokesperson for UCSF told KQED that their hospital is nearly always at or over capacity. UCSF declined 41% of the transfer requests it received in the last year.
Dr. Andrew Fenton, Queen of the Valley’s chief of staff, said the ER is not a good place for people to wait. “If you’re a sick patient, you’re trying to convalesce and you’re in the emergency department, the lights are on and there’s alarms beeping. It’s not the correct place,” he said.
Patients get stuck and get worse because there aren’t enough specialists available to offer the right care, he said, especially doctors willing to work on-call shifts inside hospitals. His hospital used to have an on-call specialist focused on ears, nose and throat.
“They’re gone now,” he said. “We don’t have ophthalmology, we don’t have plastic surgery or oral maxillofacial surgery.”
Meanwhile the emergency department is completely full. The hallway is lined with patients waiting on gurneys. One bleeds from a head injury. Another has lacerations on his face. Doctors have even transformed a small office near the waiting room into an exam room to evaluate more patients.
“It looks a little bit like a MASH unit right now,” said Fenton, referring to mobile army surgical hospitals. “When you come into the ER, it’s not pretty.”
Long wait times inside emergency departments are not new. And neither are staff shortages, but both have been exacerbated by the pandemic. Hospitals are flooded by patients who have delayed care in recent years, and there aren’t enough nurses to meet the demand. Burnout hit an all-time high during COVID, which inspired many health care workers to retire early.
“The system was broken before the pandemic,” Fenton said. “It’s in shards now.”
Even Hernandez can’t get into a clinic to see a specialist for himself — he needs to see a gastroenterologist for some preventive care. He called his health plan recently; the next available appointment is four months out.
California will have the largest physician shortages of any state in coming years, according to a 2020 study that found the state’s doctor shortage is expected to top 32,000 physician jobs over the next decade.
“It’s hard,” said Hernandez, of the California Medical Association. “It will get nothing but worse.”
The problem starts with medical school. The number of students in training is not rising fast enough to fill empty slots. Hernandez said that California has to train more doctors fast, and the state has to create more residency slots and “really start to think about this in very new and innovative ways to try to find these solutions to try to backfill those roles.”
In Butte County, there is a shortage of mental health specialists. So the city of Chico is partnering with a nonprofit to launch a new psychiatric residency program to fill the need, “to be able to just home-grow their own psychiatrists for that part of the state,” Hernandez said.
There also have to be incentives for doctors to stay in California after they finish medical training. Hernandez is pushing the state to increase loan-forgiveness programs for individuals who will serve underserved regions of the state.
“If doctors with cultural competency are inspired to work with the communities that need their expertise, it makes for a much, much better health care delivery system,” said Hernandez.
Back inside the emergency department in Napa County, the woman with pancreatitis calls for a nurse because her pain is increasing.
“It could take her days to go someplace,” said ER doctor Marks — maybe another day to find an ambulance to make the transfer.
Marks wishes there were more she could do. But she has to move on.
Her next patient waits on a gurney in the hallway.