How the Coronavirus Attacks Your Lungs
The coronavirus has had an enormous impact on our lives: how we work, communicate and congregate. At this point, we’re familiar with how to protect ourselves from the virus – and the disease it causes, COVID-19 – by washing our hands thoroughly, wearing masks and social distancing.
Most people who get the virus are mildly sick and will recover at home. For others, the virus can be severe, even fatal.
One significant way the virus attacks is deep in our lungs. Here’s how.
Viruses are simply genetic material wrapped in a layer of protein and fat. They exist in a gray zone between life and death: They’re active inside a living thing, powerless out in the open, yet rise again in another host.
“Outside the cell, the virus is basically waiting to attach to another cell,” said Dr. Melanie Ott, virologist at the Gladstone Institutes in San Francisco.
“The purpose of a virus is to persist,” Ott said. Viruses do this by infecting human cells and using them for the virus’ own purposes, basically making their host into a “little mini virus-producing machine,” Ott said. From there, new virus particles spread.
Ott said the coronavirus has found a particularly good home in humans because the virus can cause less severe symptoms in many people, sometimes even being spread by people who are unaware they are carrying it.
“It’s actually one step ahead of us, in the way that it spreads relatively undetected in some people,” she said. That allows this virus to “multiply and persist much longer than other deadly viruses.”
An individual virus particle, called a virion, is invisible to the naked eye. It would take roughly 1,000 coronavirus particles to span the width of a human hair.
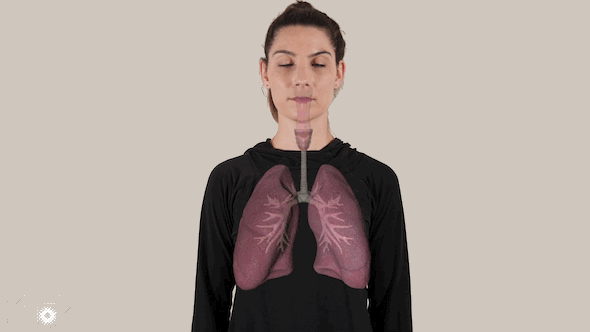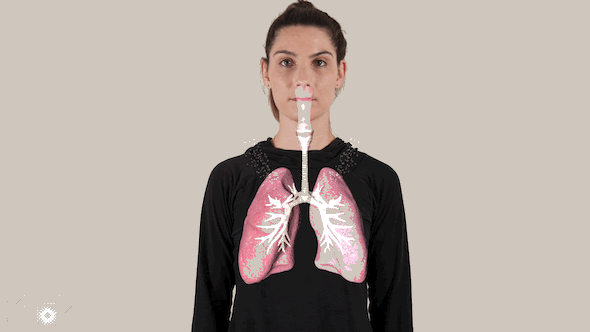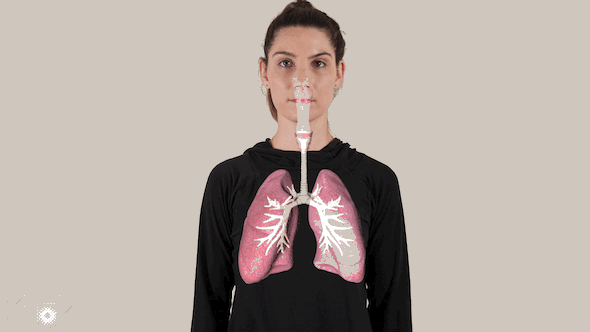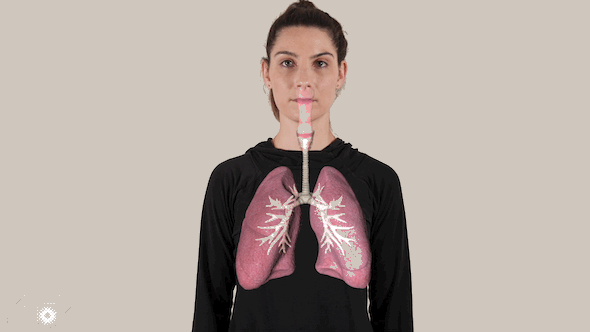
The virus spreads on moisture droplets through the air or on surfaces, eventually finding its way inside our bodies – typically through the eyes, nose and mouth.
Inside the body, the coronavirus attacks the cells in the back of the infected person’s nose, replicating and spreading downward, and infecting healthy cells along the way.
Some viruses, like those that cause the common cold, infect upper airways, including the nose and throat. Others can cause viral pneumonia that usually infects smaller areas of just one lung.
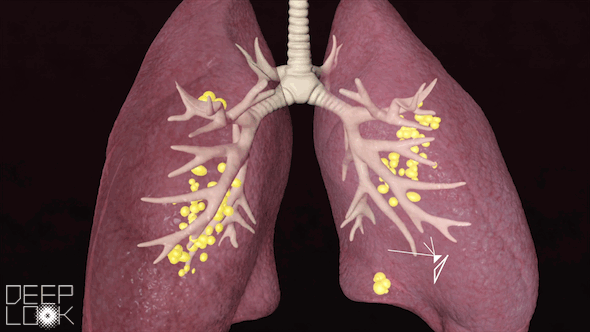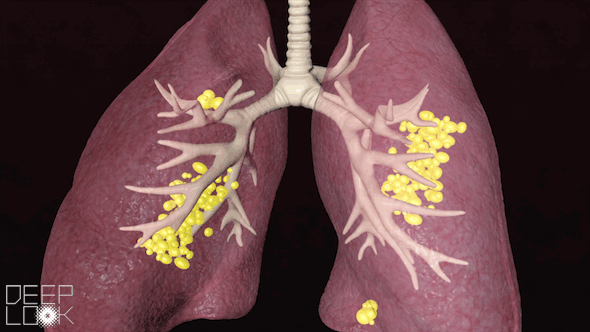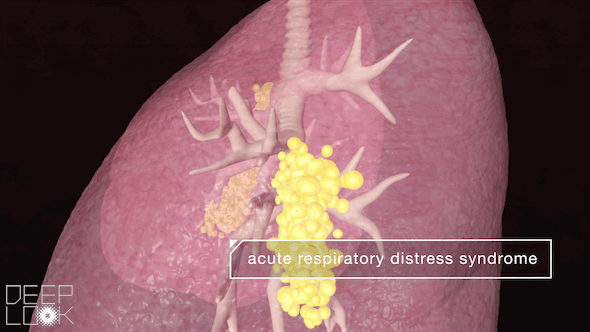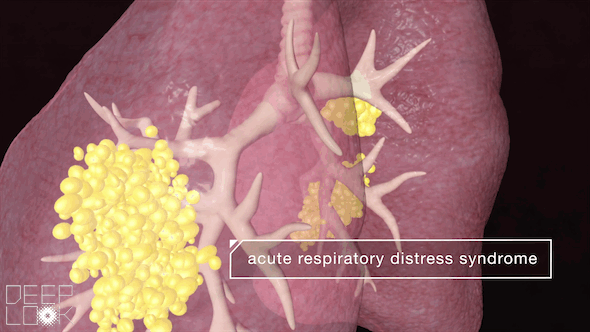
The coronavirus packs a vicious double punch: It can infect the entire respiratory system, all the way down to millions of tiny air sacs in the lungs called alveoli.
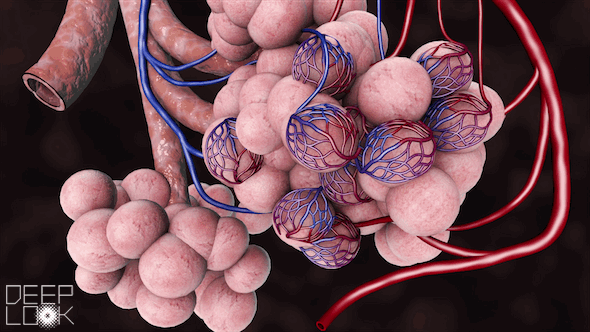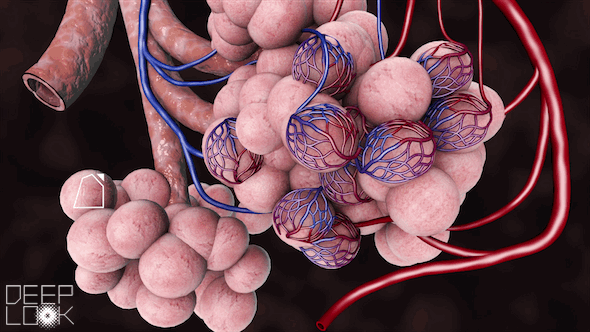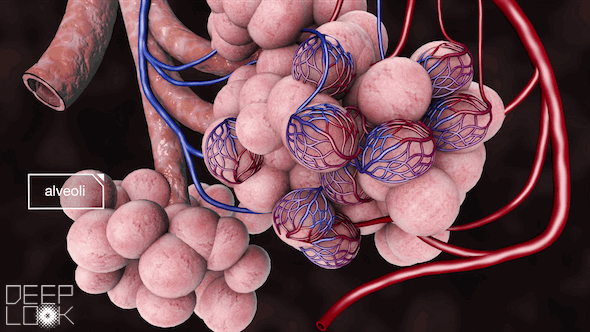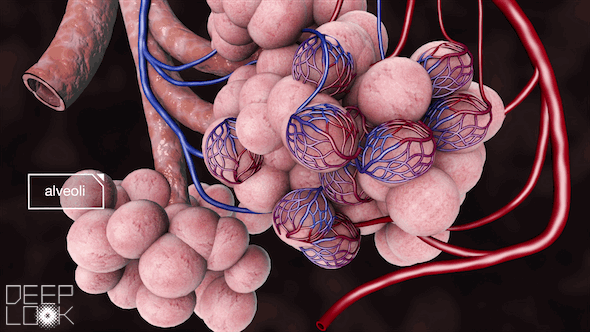
“There aren’t a lot of respiratory viruses that go both upper and lower, and this is one of them,” said Dr. Michael Schivo, a pulmonologist at UC Davis Health. “Number one, [the coronavirus] can make us sicker. And number two, it can cause low oxygen. Those are probably the two biggest problems with it.”
Alveoli make up 99% of the surface area of the lung.
“The airways are equal to a tennis racket laid on the doubles tennis court,” said Dr. Michael Matthay, a professor of medicine at UCSF. “The rest of the tennis court are the alveoli.”
The alveoli literally keep people alive by bringing oxygen into the bloodstream and excreting carbon dioxide.
But the coronavirus disrupts this process.
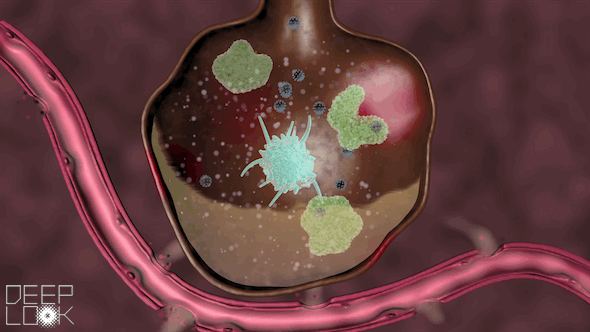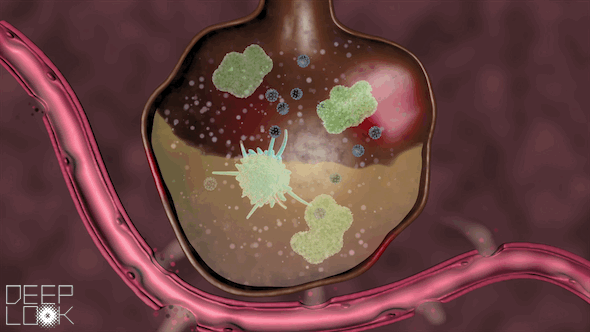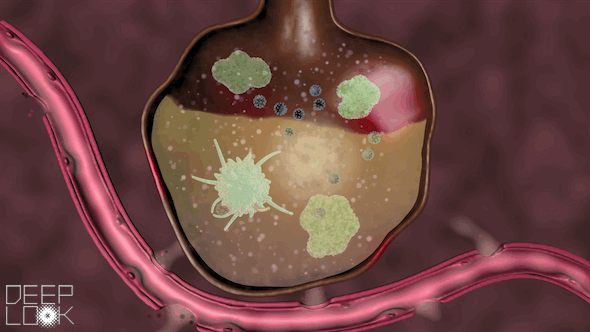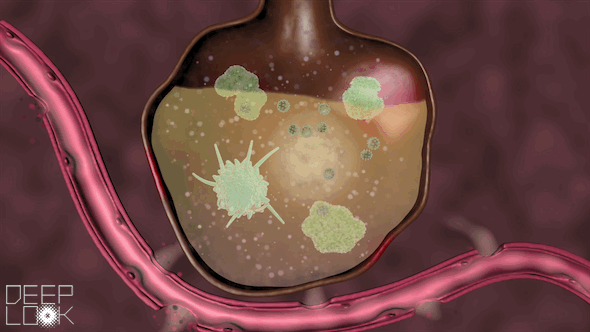
When the virus particles enter the alveoli, they continue to replicate, injuring the lungs.
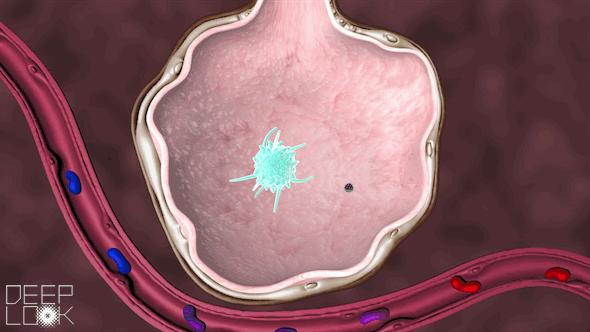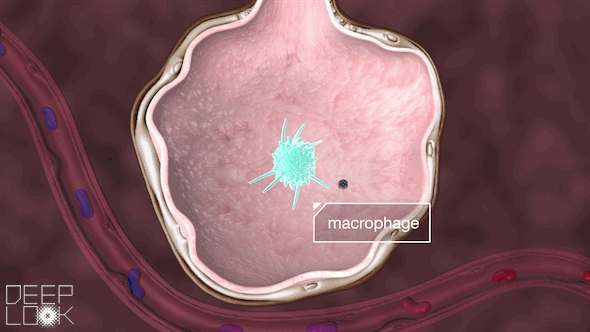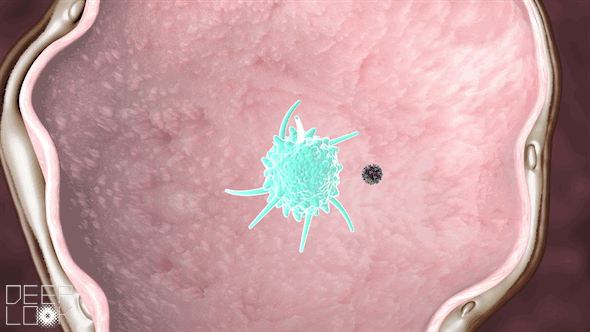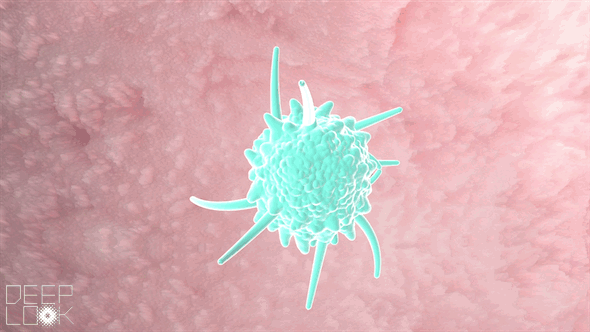
Inside the alveoli are immune cells called macrophages, which act as sentinels for the lungs. They’re “waiting to fight off the cigarette smoke, or pollution or anything else,” Matthay said.
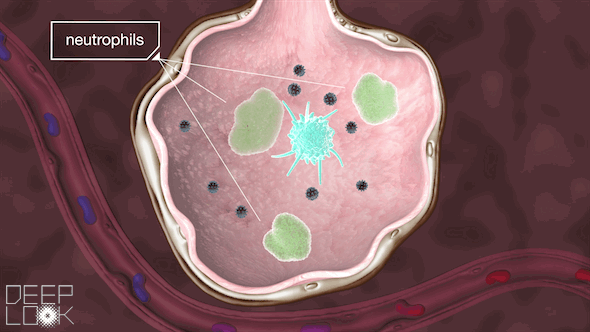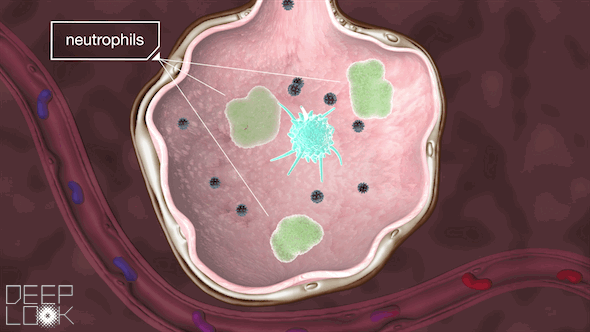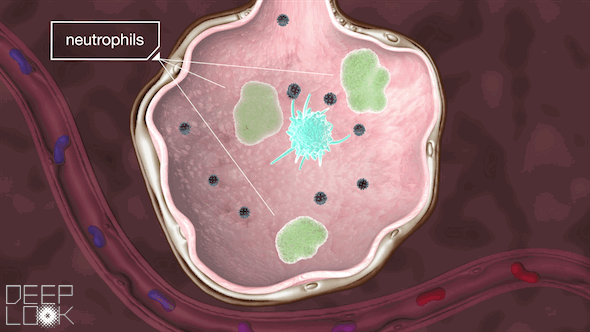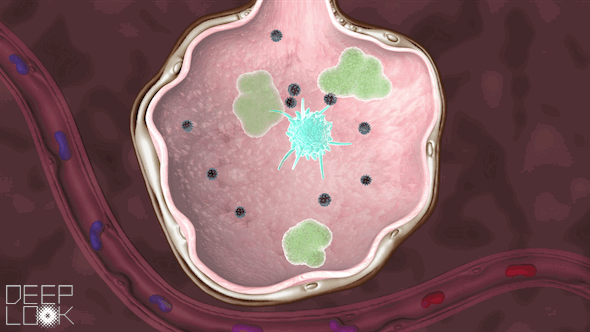
These macrophages attack the virus, a battle that the immune system sometimes wins.
“They’re what we call the first responders,” Schivo said. “They recognize danger, and they try to get rid of it.”
If our body needs more help, it recruits more immune cells, called neutrophils. Sometimes, however, during the battle, the immune system goes haywire. It throws relentless resources at this unrecognizable virus, and that can wreak more havoc than repair. This immune system overreaction is called a cytokine storm.
This two-pronged attack – from the virus and from our immune system’s explosive response – makes the coronavirus so deadly.
In the worst-case scenario, the walls of the alveoli begin to break down.
Fluid rushes from the blood vessels into the alveoli, filling them up and blocking the exchange of gases. When this happens, we can’t excrete enough carbon dioxide, nor absorb enough oxygen. It becomes much more difficult to breathe.
These lung injuries can lead to acute respiratory distress syndrome (ARDS), a condition when fluid fills many alveoli on both sides of the lungs. ARDS is what most people with COVID-19 die from.
“When someone develops ARDS and if it’s severe, their mortality is 40%,” Schivo said.
To ultimately beat this coronavirus, humanity will need a very effective antiviral medication or, better yet, immunity through a vaccine.
While the impact from this pandemic has been devastating, we can learn from it, scientists say, so we can stay a step ahead of the next one.
“There’s no reason to think we can’t generate a vaccine,” said Luis P. Villarreal, professor emeritus at the School of Biological Sciences at UC Irvine. “Then it will be controlled just like measles was and it can be eradicated if you choose to really implement it on a large scale. It would be difficult, but it could be eradicated.”
Reporting contributed by Gabriela Quirós, Deep Look coordinating producer, and Annie Roth, Deep Look intern.

