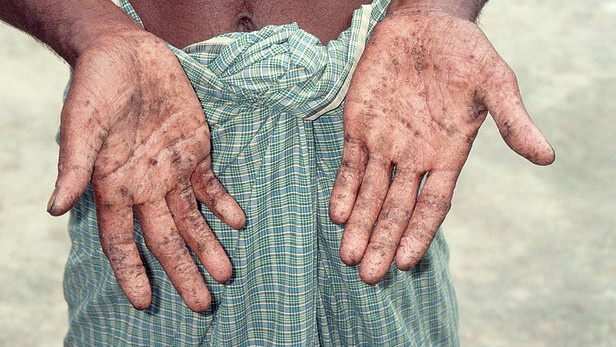
(In a highly controversial move, the Bush White House postponed the revised rule, approved during the Clinton years, and asked the academy to evaluate new studies on arsenic’s health effects. To the dismay of some Bush supporters, the new studies actually strengthened the evidence.)
Arsenic levels in most groundwater samples in the United States average 1 ppb or below. But some places in the West, including the San Joaquin Valley, exceed 50 ppb. Small communities like those in the valley often get their drinking water from groundwater wells (while cities use surface water), and so are more likely to have higher concentrations of arsenic in their water supply.
About 30 million California residents rely on groundwater supplied by community water systems for at least some of their drinking water, according to the California Department of Public Health. Demand for groundwater increases during droughts, when surface water supplies start drying up.
A report released by the State Water Resources Control Board last month found that 21 million residents get their drinking water from community water systems with contaminated groundwater sources. Arsenic was the most common naturally occurring contaminant, followed by nitrates.
The water board identified three general approaches to solving the problem: preventing pollution, removing contaminants, and finding alternative water supplies. Unfortunately, there’s no economically feasible way to remove a naturally occurring contaminant like arsenic from groundwater. In that case, the board noted, water suppliers should focus on finding alternative supplies or treatment at the point of delivery.
But the board also acknowledged that community water systems in rural areas, which often serve just a few thousand people, can’t afford any of these solutions and may face persistent contamination problems.
The EPA recognized that many smaller, poorer community water systems might not be able to meet the tougher standard. That’s why it extended the compliance deadline to January 2006. Yet today some water systems still lack the technical and financial means to comply, prompting regulators to suggest exemptions, including stop-gap measures like supplying bottled water, to give them even more time.
But as Balazs and her colleagues argue, this would simply perpetuate the inequities they found. Small systems often lack the economies of scale to raise rates and the know-how to apply for loans to hire experts who can install and oversee new treatments. And their customers have to buy bottled water so their families have safe drinking water at home—whether they can afford it or not.
If the EPA simply extends the compliance period, it risks creating a situation where community water systems that can’t afford treatments will continue to violate the arsenic safety standard. And customers too poor to buy bottled water will suffer chronic exposure to arsenic.
To address these disparities in the short term, Balazs and her colleagues argue, regulators must provide technical and financial assistance tailored to the special needs of small water systems so they can reduce their arsenic levels. But in the long run, regulators will need to help these communities tap into regional systems so they can absorb the high costs of delivering safe drinking water to everyone in the valley.
Only then will public health advocates be able to celebrate the victory they envisioned more than a decade ago.