Odds are that you know someone who’s had a heart attack. One American suffers a coronary event every 25 seconds and about every minute someone dies from one.
Doctors thought they understood artery-hardening diseases, such as atherosclerosis, that lead to heart attacks, strokes and death. But these generally accepted theories are contradicted by new research performed at the University of California, Berkeley. According to a new study published in Nature Communications, a previously unknown type of stem cell is actually the underlying cause for clogged arteries.
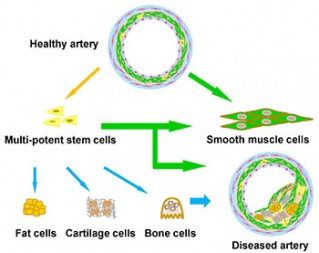
For decades, scientists believed that heart disease was caused by the smooth muscle cells that line artery walls. It was thought that bad (LDL) cholesterol damaged the arteries and triggered smooth muscle cells to rapidly reproduce. This led to a build up of fibrous scar tissue that narrowed and hardened the arteries, restricting blood flow. As a result, most therapies focus on physically widening the inside of the blood vessels or replacing the damaged area with a graft.
These beliefs are challenged by new research performed by principle investigator Song Li, a professor of bioengineering and researcher at the Berkeley Stem Cell Center, and his colleagues.
“For the first time, we are showing evidence that vascular diseases are actually a kind of stem cell disease,” said Song Li in a university news release. “This work should revolutionize therapies for vascular diseases because we now know that stem cells rather than smooth muscle cells are the correct therapeutic target.”