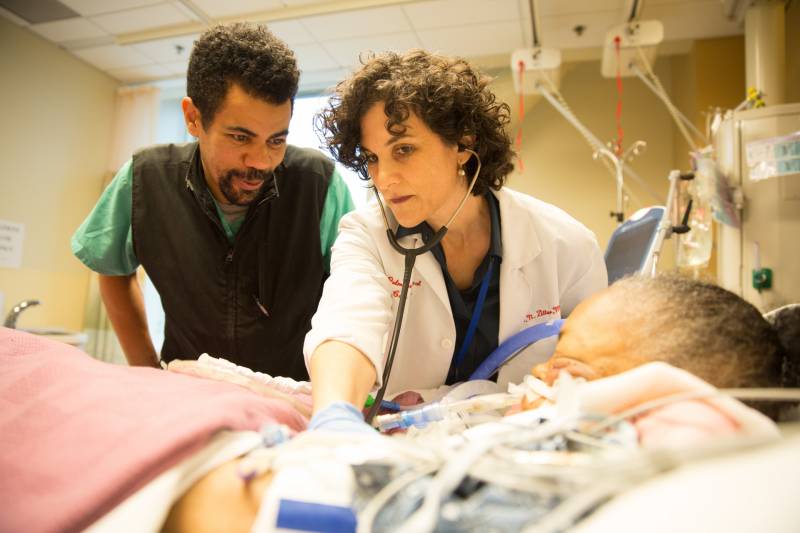
Dr. Jessica Zitter specializes in critical and palliative care medicine and practices at Highland Hospital in Oakland, where she helps people with serious illness talk about how they want to live, all the way to the end.
Zitter says those are conversations we all should be having with our loved ones — even if we’re healthy and young. She is the author of Extreme Measures: Finding a Better Path to the End of Life, and her work has been featured in the documentary “Extremis” on Netflix, as well as the forthcoming film “Caregiver: A Love Story.”
Here are three stories about her patients, followed by some concrete tools you can use for planning and talking about the end of your life with loved ones.
Michael Thomas: ‘Enjoying Every Moment’
Michael Thomas is 64 and has COPD, a lung disease that makes it hard to breathe. He has already been in and out of the hospital several times this year and is particularly vulnerable if he were to get sick with COVID-19.
When Zitter talked with him over Zoom this spring, she asked him what he wanted most. His answer? To be with his children and grandchildren in Ohio. But he also said he didn’t feel a sense of urgency to visit them, because he believed he had plenty of time left.

“You are a more confident person than I am about myself!” Zitter told him. “I want to be totally frank with you, because I think you deserve that. I’m concerned you may not have as much time to live as you think you do. If someone told me, ‘Michael is going to die within the next six months,’ I would not be surprised.”