Five o’clock p.m. at the park near Duboce Triangle in San Francisco is canine happy hour. About 40 dogs are running around, chasing balls, wrestling each other, as their owners coo and '90s hip-hop bumps out of a portable speaker.
It's Not Just Doctors and Nurses. Veterinarians Are Burning Out, Too
One chihuahua mix named Honey lounges on a bench wearing blue Hepburn sunglasses, a blue tutu and a string of pearls. Her owner, Diana McAllister, feeds her treats from a blue plastic bag, then pops one into her own mouth.
“We have turkey jerky,” she says. “I make her food. It’s a raw diet with steamed vegetables and a little brown rice. And then little turkey treats.”
One of the well-worn facts about San Francisco is that there are more dogs in the city than children. And after spending two years at home through the pandemic, it’s clear that for a lot of these owners, their dogs are their children.

“I always say, dogs are people, so I love him,” says Yves Dudley, looking on as her 9-month-old collie-schnauzer mix plays in the grass.
Most of the dogs out today are under age 2: pandemic puppies. Across the country, 23 million American families adopted a new pet in the first year of the pandemic. Others quickly became intimately familiar with their existing pets’ daily routines, noticing abnormally frequent vomiting, urinating or coughing that was easy to miss while working away from home. The spike in pet health concerns has been putting a strain on a corner of the medical world that is often overlooked: veterinarians.
Dog owners in Duboce Park say they’ve had to wait months for vet appointments or drive to Walnut Creek or San Bruno to get care.
“Getting your dog in to see the vet is as competitive as trying to buy Coachella tickets online,” says Laura Vittet, whose golden retriever, Gertrude, is a year and a half. “You have to wait by the phone, you have to be ready to refresh your browser. It's a very intense experience.”
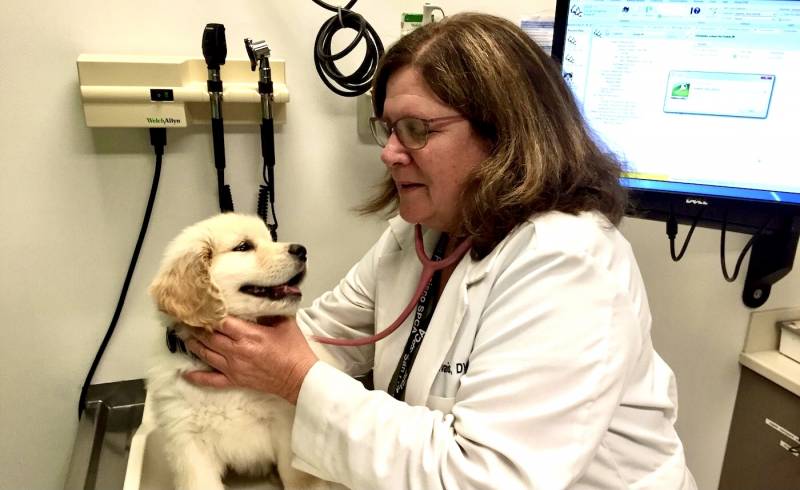
The overwork and short staffing of the pandemic has affected veterinarians as much as it has other doctors and nurses, and dealing with the constant moral dilemmas and emotional output is driving many to burn out. At the SPCA on Fillmore Street in San Francisco, so many vets and technicians were leaving that they had to cut back their clinic hours, says veterinarian Kathy Gervais.
Gervais walks through the ICU, checking on one dog waking up from anesthesia and another recovering from cardiac surgery. She works 12-hour days, constantly zigzagging from new puppies to dying cats. They euthanize about five animals every day, she says. And the whole time, she has to take care of the humans, too.
“To these people, and especially in these times, this is their love,” she says, thinking especially of the owners who dress and coif and cook for their dogs. “This is their being, this is what they live for. And for vets, it's very hard for us to draw the line.”
Even before the pandemic, vets’ mental health was suffering from empathy overload and compassion fatigue. They carry the weight of having to euthanize animals that could be saved, but their owners can’t afford the care. Some upset owners become downright abusive, berating vets or later bullying them online.
“I dare you to try to talk to a veterinarian who's been in practice more than five years who doesn't know somebody who has committed suicide,” says Gervais. “I, unfortunately, can count on more than 10 fingers: classmates, colleagues, people I've dated.”
One out of six veterinarians has considered suicide, according to studies from the Centers for Disease Control and Prevention. While male vets are 1.6 times more likely to die by suicide than the general population, female vets are 2.4 times more likely, and 80% of vets are women. The most common means is euthanasia drugs.
In the early months of the pandemic, Gervais could see things were getting worse. She helped organize the Veterinary Mental Health Initiative, which offers free support groups and one-on-one help to vets across the country.
All the facilitators have doctorate-level training, says founder and director Katie Lawlor, also a psychologist, and they’re all familiar with the issues troubling vets.
“Burnout, compassion fatigue, managing panic attacks, and how to communicate with both supervisors, colleagues and clients when you're under extreme deadlines or very intense stress,” she says. “And, the loss of their own companion animals.”

The initiative helped Razyeeh Mazaheri work through the anxiety she was feeling every day caring for animals at a clinic outside Chicago last year. The clinic was regularly double or triple booked. As a new vet — Mazaheri graduated from vet school last spring — juggling so many cases was terrifying.
“I just feel like if I make a mistake, that is a problem. And if I make a mistake and kill something, that is my fault,” she says, tearing up. “I just knew that I was burned out.”
Through the support groups, Mazaheri was able to see that others shared her concerns and she learned tools for managing them. The initiative, housed under the nonprofit Shanti Project, has groups specifically for emergency vets, vet technicians, recent grads, like Mazaheri, and longtime vets, like Kathy Gervais, who have more than 20 or 30 years of experience.
“I've had people look at me sometimes when they've seen me really tired, going, ‘Kathy, walk away,’” Gervais says.
“I'm not ready to do it because, bottom line, I love my job. It is a vocation. It is a passion. And it's hard to walk away from that,” she says. “But if it's going to kill me on the flip side, I would hope I could just say, ‘OK, that's it. I'm done.’”
If you or someone you know is considering suicide, please call the National Suicide Prevention Lifeline: (800) 273-TALK (8255).